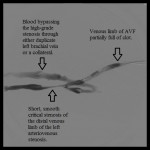
- Fistulagram before interventions showing stenosis of the distal left brachial vein.
- Waist around a balloon dilating the stenosed segment of the distal left brachial vein.
- Fistulagram after first balloon dilation of the stenosis in the distal left brachial vein.
- Fistulagram after second and final dilation of the stenosed distal left brachial vein.
- Final fistulagram of the AVF showing the proximal left brachial vein and the distal left brachial artery.
I use this case to illustrate when to end an intervention and avoid harming the patient. “Better is the enemy of good” is a truism among interventional radiologists. In trying to improve the outcome of an intervention by doing more, terrible things may happen and foul earlier efforts.
This was a patient with a failed arteriovenous fistula (AVF) between the proximal left brachial vein and the distal left brachial artery. Pullback venogram recorded from the central veins to the mid left brachial vein revealed normal central veins, a smooth, short critical stenosis of the distal left brachial vein, and clot in the proximal left brachial vein.
After pharmachomechanically clearing the thrombosed proximal segment of the venous limb of the fistula, I used a non-compliant balloon to dilate the distal stenosis. It is conventional to oversize balloons for venoplasty by 10% to 20% in recognition of the odd behavior of the scar tissue and abnormal smooth muscle encircling the strictured venous segment, at the same time being careful to avoid rupturing the vein during the inflation. It is common knowledge that the shadow of the lumen of the treated segment is often cosmetically unappealing soon after angioplasty and there is urge to improve such appearance by inflating the segment with larger balloons. It is not uncommon that such zeal is rewarded with a tear or rupture of the vein.
If this happens one may do one of a few things:
- They may tamponade the bleeding by inflating a balloon across the tear for a few minutes. This may be sufficient, but risks re-thrombosing the proximal segment of the vein if it has already been cleared of clot. In fact this is one reason some interventionists address downstream venous stenoses before clearing clot in the proximal venous limb.
- If balloon tamponade does not stop the bleeding, the access can be intentionally re-thrombosed by compressing the portion of the vein (or graft) proximal to the tear. This should be a last resort and should be done only when isolating the injury with a covered stent is infeasible.
- If a covered stent is available and balloon tamponade of the tear has failed, the tear may be isolated from the circulation with a covered stent.
It is preferable to avoid such complication by accepting some irregularity and residual stenosis (<30%) of the vein after angioplasty, recognizing that some of the spasm is physiologic response to the balloon inflation that resolves on its own or after intravenous injection of nitroglycerin. In addition, noting the presence of certain features that prove adequate intervention may be reassuring reason to end the procedure. These include:
- Resolution of collaterals associated with the stenosis before the intervention(s).
- Palpating a pulse or feeling a thrill where none was present before.
- Observing improved rate of venous flow on the post-intervention examination relative to the pre-intervention examination.